Back to Annual Meeting Program
Use of CT Angiography and CT Perfusion Imaging in the Selection of Hyperacute Stroke Patients to Undergo Emergent Carotid Endarterectomy Versus Intra-Cranial Thrombectomy
Grant R Major, Mark W. Fugate, Thomas G. Devlin, R. Kent Hutson
University of Tennessee College of Medicine Chattanooga, Chattanooga, TN
BACKGROUND - Patients with acute stroke symptoms due to carotid disease are typically not considered for emergent carotid endarterectomy (CEA) due to the risk of fatal intracranial hemorrhage secondary to reperfusion injury. Past studies have failed to show consistent benefit of early operative intervention, presumably due to a high rate of unrecognized intracranial thromboembolism. The emergence of neuro-endovascular clot retrieval has revolutionized acute stroke treatment since initial device clearance by FDA in 2004. While approximately 1 in 10 patients in the national registry undergoing emergent intracranial embolectomy required simultaneous carotid revascularization (typically angioplasty), this ratio increased to approximately 1 in 3 for patients in the southern Stroke Belt. In this setting, a small, but well defined, population of patients has emerged that present with severe acute stroke symptoms due to critical carotid stenosis or occlusion without intracranial thromboembolus. Based on the recent radiology techniques utilized by endovascular stroke specialists, this case report describes how Computed Tomography (CT), cervical and cerebral CT angiography (CTA), and CT perfusion (CTP) imaging can be used to emergently recognize stroke patients without intracranial thromboembolism who are candidates for emergent surgical carotid revascularization.
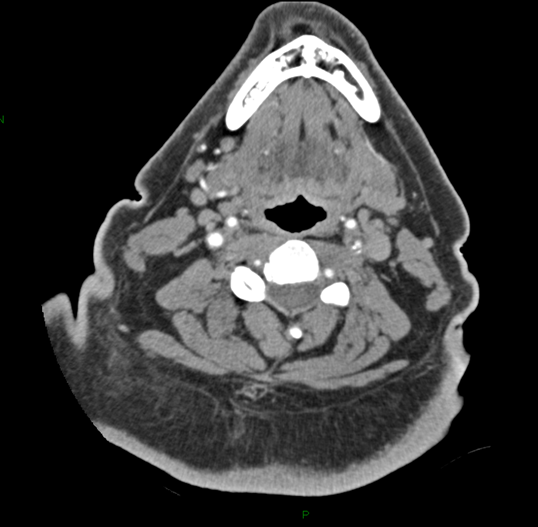
METHODS - As done routinely in all stroke patients, non-enhanced CT imaging is first performed to rule out intracranial hemorrhage and other CNS pathology that would contraindicate emergent therapy. Next, CTP is performed allowing discrimination of potentially reversible brain ischemia from irreversible brain injury. CTA of the head and neck is then performed to identify thromboembolus location in the extra-cranial carotid system, the intra-cranial circulation, or both. Based on this imaging, patients with isolated extra-cranial carotid lesions with potentially reversible brain ischemia may be identified. By correlating the patient’s symptomatology with detailed imaging data, the surgeon can best assess risk-benefit ratio and select those patients properly suited for emergent CEA.
RESULTS - We describe a case in which emergent CEA was performed to achieve symptomatic resolution in a patient experiencing a massive stroke-in-evolution. Importantly, the utilization of CTP is illustrated to identify salvageable ischemic penumbra in this patient, thus influencing the decision to proceed with surgery. Once viable brain tissue was confirmed, the patient was immediately taken to the operative theatre for emergent CEA, and dramatic improvements were observed postoperatively.
CONCLUSIONS - We conclude that emergent CEA is indicated in select patients presenting with acute stroke-like symptoms. CTP, in conjunction with CT and CTA, helps delineate patients with salvageable brain tissue and should be used in the initial work-up of these patients. Rather than adhering to strict time frames, we advocate the utilization of CT-CTA-CTP in the diagnosis and decision-making process regarding markedly symptomatic stroke patients who are potential candidates for emergent CEA. 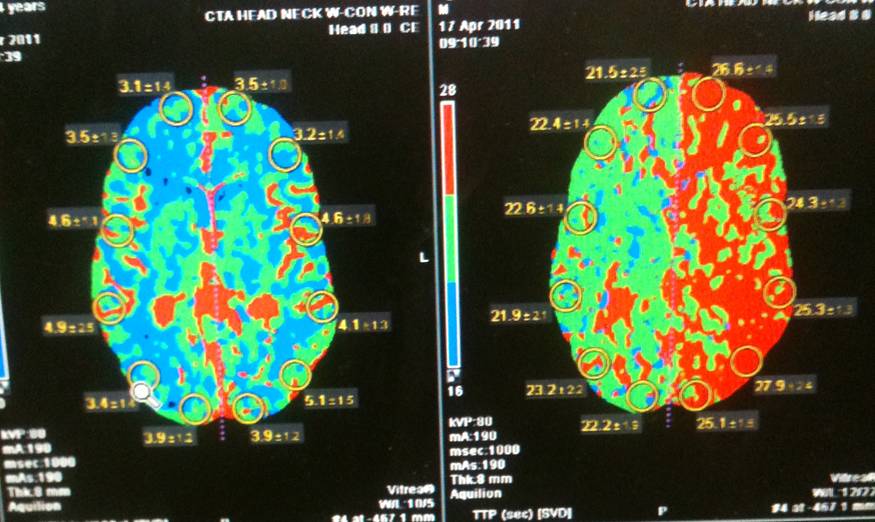
Back to Annual Meeting Program
