Back to Annual Meeting Program
Managing Severe Upper Extremity Ischemia from Mobile Aortic Arch Thrombus: A Novel Approach Using Isolated Limb Perfusion with Tissue Plasminogen Activator
Ramyar Gilani, Peter I. Tsai, Matthew J. Wall, Jr., Peter H. Lin
Baylor College of Medicine, Houston, TX
INTRODUCTION:
Etiologies of upper extremity ischemia are numerous and include embolic aortic pathology. Traditional operative management for this entity includes open thrombectomy, catheter directed thrombolysis and/or percutaneous mechanical thrombectomy. These conventional options, however, may not be ideal for patients having unstable aortic arch thrombus and profound distal arterial thrombosis of the hand. An alternative approach for such patients is isolated limb perfusion (ILP) with tissue plasminogen activator (tPA).
METHODS:
A 37 year old female presented with sudden onset acute left hand ischemia associated with sensory and motor deficits. An axillary pulse was present and distal pulses were absent as were radial, ulnar and palmar signals. Her medical history was unremarkable but she was a 1 pack/day smoker. Her evaluation included a chest CT-angiogram showing a pedunculated aortic arch thrombus that was confirmed on transthoracic echocardiogram (TTE) and was mobile (Figure 1). Her hand ischemia was presumed to be caused by an embolus originating from the aortic arch.
RESULTS:
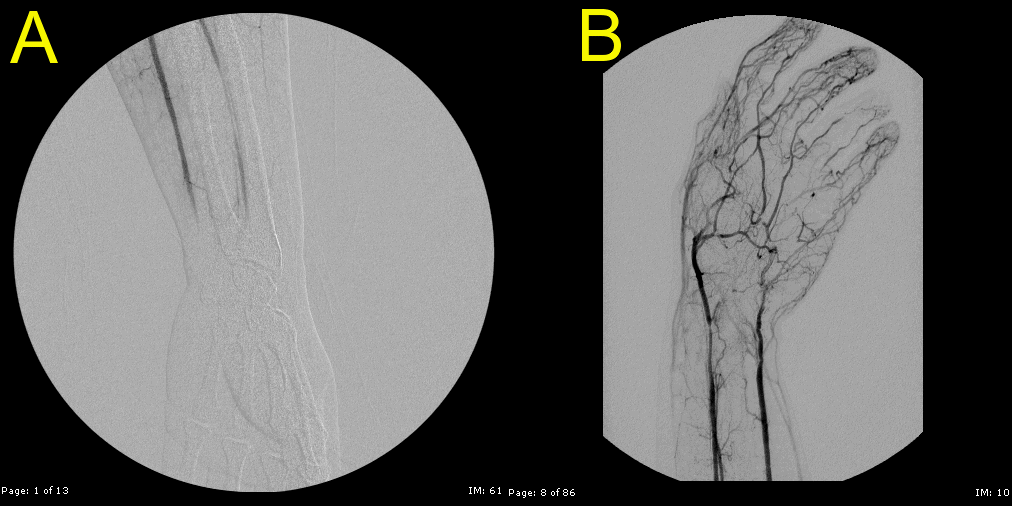
Given the severity of distal forearm and hand ischemia with the presence of mobile aortic thrombus, catheter directed thrombolysis was felt to be contraindicated and the patient was taken to the operating room (OR) for emergent brachial, radial and ulnar thrombectomy. This yielded some thrombus; however, an intraoperative angiogram (Figure 2A) post-thrombectomy still showed significant residual hand thrombus with absent radial, ulnar and palmar signals. Further thrombectomy was felt to be ineffective and ILP with tPA was felt to be most appropriate. A perfusion circuit was constructed and connected to the patient via brachial artery and vein cannulas. A proximal arm tourniquet was placed. The perfusate was charged with 25 mg tPA/hour for a total circulation time of 2 hours at a flow rate of 200 cc/min. Fibrinogen levels remain unchanged during perfusion. After completing perfusion, a repeat angiogram (Figure 2B) was performed showing marked thrombus resolution. The cannula sites and incision were closed. The patient then underwent left postero-lateral thoracotomy and open aortic thrombectomy without cardiopulmonary bypass. At 6 months follow-up, radial and ulnar pulses are present and without sensory or motor hand deficits.
CONCLUSIONS:
Prompt open surgical thrombectomy remains first line therapy for cases of acute severe upper extremity ischemia due to thromboembolism although it may be ineffective for distal arterial bed thrombus. Alternatively, catheter-directed thrombolysis is effective for distal bed thrombus. However, this is precluded in advanced ischemia and when systemic tPA exposure is contraindicated due to risk of further embolization from proximal thrombus. ILP with tPA allows for rapid distal bed thrombolysis while theoretically limiting systemic exposure. In circumstances where perfusion circuits are readily available, it is possible to utilize ILP with tPA as an alternative strategy when conventional treatment methods are deemed to be suboptimal. 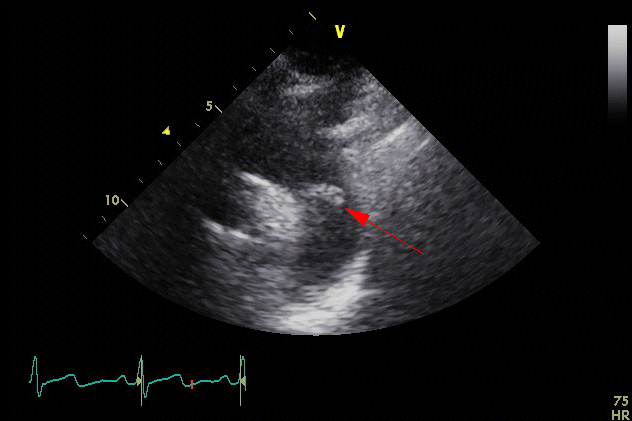
Back to Annual Meeting Program
