Impact of Suprarenal Neck Angulation on EVAR Outcomes
Asma Mathlouthi, Satinderjit Locham, Hanaa Dakour Aridi, James H Black, Mahmoud B Malas
The Johns Hopkins University, Baltimore, MD
Background: Hostile infrarenal proximal neck (β) anatomy of abdominal aortic aneurysm (AAA) has been associated with increased risk of aneurysm-related complications after endovascular repair (EVAR). However, there is a paucity of literature addressing the suprarenal angle (α). The aim of this study is to evaluate short and long-term outcomes after EVAR in patients with severe suprarenal neck angulation (>60).
Methods: A retrospective review of the medical records of 501 patients who underwent EVAR between January 2005 and December 2017 was performed. High-resolution computed tomography images of 462 (92.2%) patients were available. Patients were grouped into angulated ( α > 60°) and non-angulated ( α ≤60°) groups. The primary endpoint was freedom from type IA endoleak. Secondary endpoints included 30-day mortality, long-term survival, primary clinical success and freedom from aneurysm rupture and graft migration. Primary clinical success was defined in according to SVS guidelines as clinical success without the need for an additional or secondary surgical or endovascular procedure.
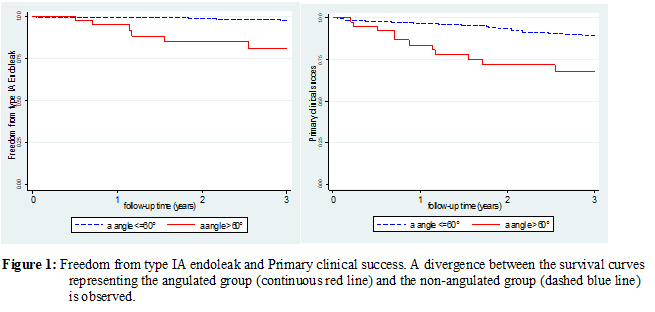
Results: Out of 462 patients, 47 (10.17%) were included in the angulated group (α>60°). Median follow-up time was 33 months (IQR 14-55).Compared to patients in the non-angulated group, those in the angulated group had larger neck diameter at the level of the renal arteries [mean(SD): 25.8(3.8) vs. 24.6(3.4) millimeters, p=0.029] and increased infrarenal angle (β) [mean(SD): 50.1(22.6) vs. 41.7(23.9) degrees, p=0.02]. The 3-year freedom from type IA endoleak estimates were 80.9% for the angulated group compared to 97.9% for the non-angulated group (p<0.001). The angulated group showed significantly higher 30-day mortality (12.8% vs. 0.5%, p<0.001). On the other hand, the 3-year results showed that patients in the non-angulated group had higher rates of primary clinical success (89% vs. 68.1%, p<0.001), freedom from rupture (99% vs. 97.2%, p=0.02), freedom from migration (100% vs. 92.6%, p<0.001) and long-term survival (91.4% vs. 75.2%, p=0.003) compared to those in the angulated group. After adjusting for age, gender, neck diameter and infrarenal angle (β), severe suprarenal neck angulation was associated with higher odds of type IA endoleak [aHR(95% CI): 8.8 (2.9-26.6)], loss of primary clinical success [aHR(95% CI): 4.4 (2.4-7.9)] and 30-day mortality [aOR(95% CI): 29.4 (5.3-162)] compared to α≤60° (All p<0.001) .
Conclusion: This is the first report to show a significant increase in operative mortality in patients undergoing EVAR with severely angulated suprarenal neck. Patients who survive the operation are at increased risk of secondary interventions. These findings suggest that EVAR should be used with caution in patients with severe α angulation and underpin the role of close follow-up in this particular population. 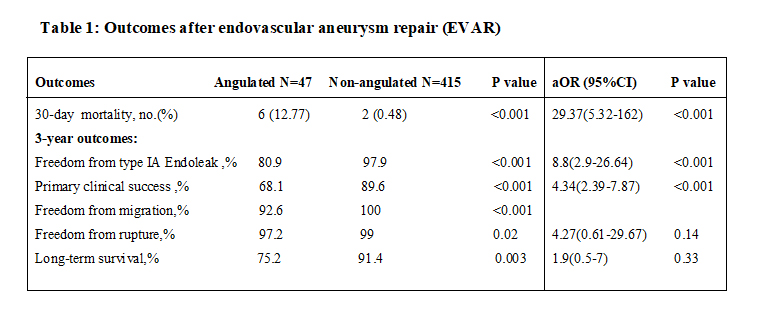
Back to 2019 Abstracts
