Performance of Viabahn Balloon Expandable Stent (VBX) Compared to Self-Expandable Covered Stents(SES)for Fenestrated-Branched Endovascular Aortic Repair.
Fernando Motta, Frederico E. Parodi, Jason R. Crowner, Luigi Pascarella, Katharine L. McGinigle, William A. Marston, Melina R. Kibbe, Mark A. Farber
University of North Carolina - Chapel Hill, Chapel Hill, NC
Introduction: The objective of this study is to compare the performance between Viabahn balloon-expandable stent (VBX) and self-expandable covered stents (SES) (Viabahn and Fluency) used as bridging stents for directional branches during F-BEVAR of complex aortic aneurysms (CAA).
Methods: Patients with thoracoabdominal aortic aneurysms (Type I-IV) or pararenal aortic aneurysms unsuitable for either open repair or endovascular repair with commercially available devices were prospectively enrolled into a physician-sponsored investigational device exempt trial. Descriptive statistics of the cohort included demographics, risk factors, as well as anatomic and device characteristics. Individual branches were grouped as either VBX or SES and were analyzed for primary patency, branched-related type I/III endoleaks, branch-instability, branch-related secondary intervention, and branch-related aortic rupture or death. Categorical variables were expressed as total and percentage, and continuous variable as median (interquartile range [IQR]). Kaplan-Meier curves were used to estimate long-term result. Groups were compared with the log-rank test. P-value <0.05 was considered statistically significant.
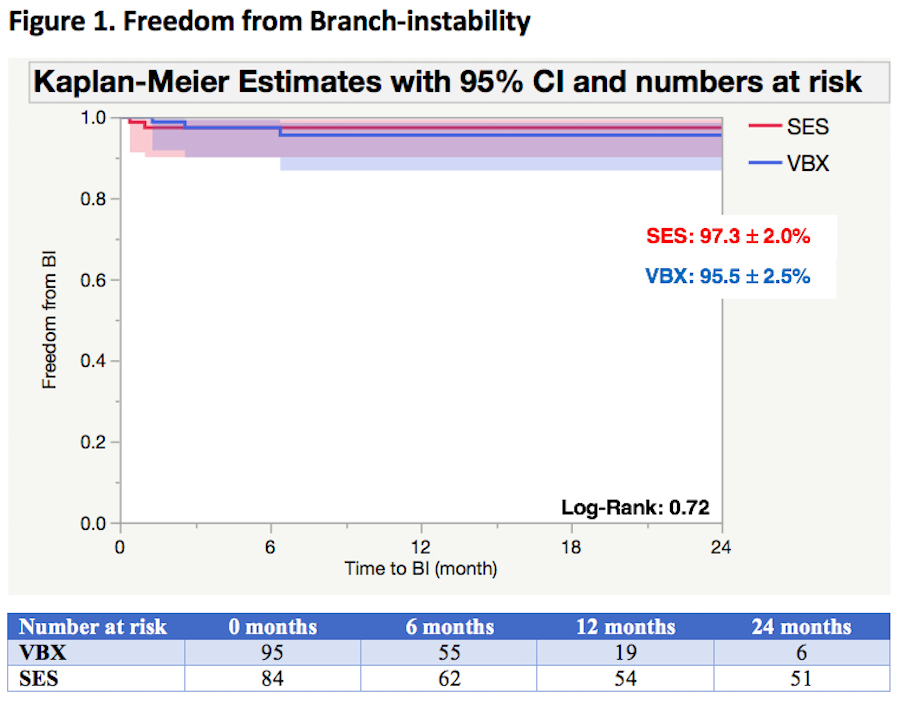
Results: During the period from July 2012 thru April 2020, 263 patients were treated for CAA with F-BEVAR. The devices used were either a custom-manufactured device (CMD) or off-the-shelf p-branch or t-branch Cook devices. The median age was 71 (IQR 66-79) years old, 70% male and 81% Caucasians. The most common cardiac risk factors were smoking (92%), hypertension (91%), hyperlipidemia (78%) and COPD (52%). The total number of vessels incorporated to repair was 977, with branches representing 18.4% (179 branches). Among the 179 branches: 54 (30%) celiac artery (CA),56 (31%) superior mesenteric (SMA), 38 (21%) right renal (RRA) and 31 (18%) left renal (LRA). VBX and SES groups represented, respectively, 53% (n=95) and 47% (n=84) of total (table I).The overall cohort survival rate at 24 months was 78.5+ 3%. There was no branch-related rupture or mortality. Primary patency at 24 months (VBX 98.1%, SES 98.6%, log-rank=0.98), freedom from endoleak (VBX: 97.3%, SES: 98.6%, log-rank: 0.63), from secondary intervention (VBX: 91.5%, SES 95%, log-rank: 0.69) and from branch-instability (VBX: 95.5%, SES: 97.3%, log-rank: 0.72) were all similar between groups (Figure 1).
Conclusion: The initial experience with VBX stents demonstrated excellent primary patency and similarly low rates of branches-related complications and endoleaks with no branch-related aortic rupture or death. Our results demonstrate that, in high volume and experienced aortic center, the VBX stent is a safe and effective bridging stent option during branched endovascular aortic repair. Multicenter studies with longer follow-up are necessary to validate our initial results. 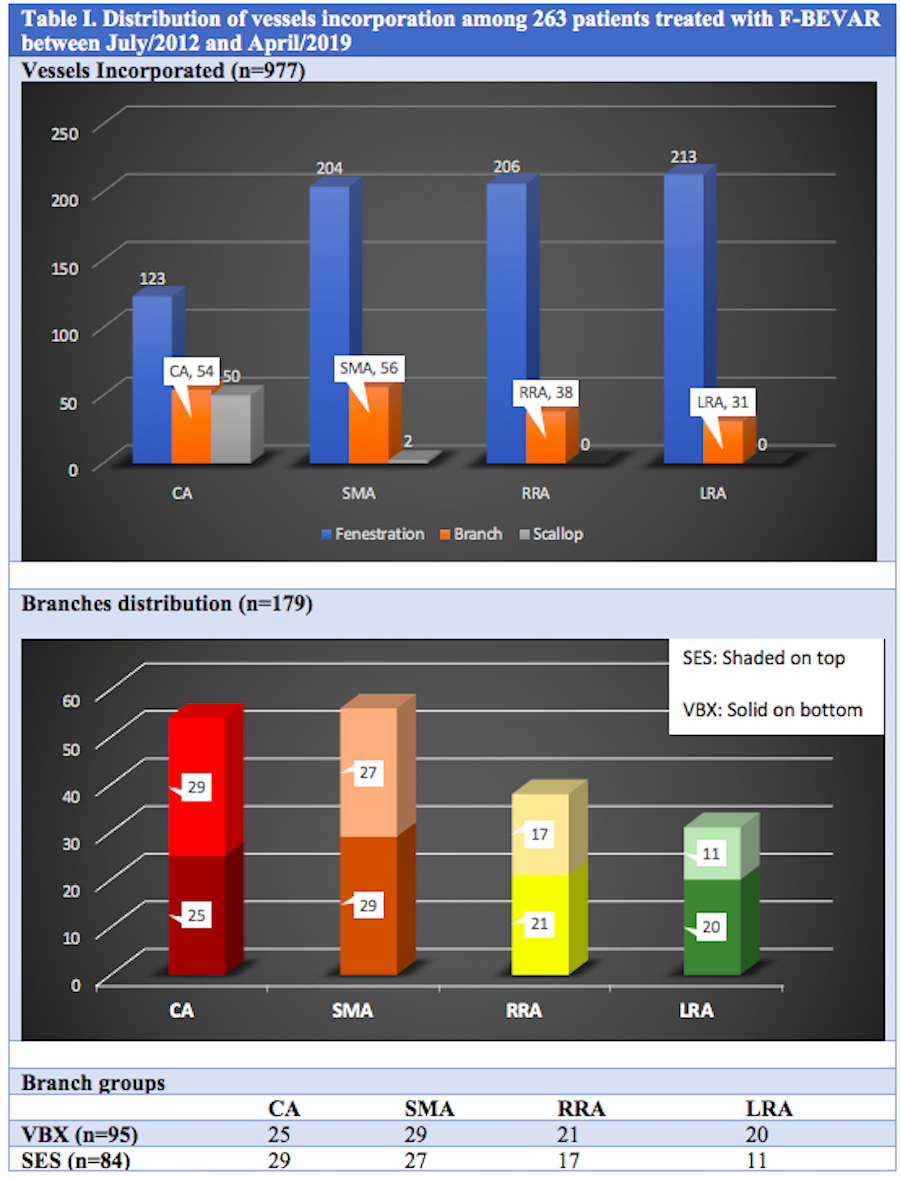
Back to 2020 Abstracts
